Other skin lesions in the newborn
Please note: images that have a white symbol at the top right, such as the Icthyosis image below, indicates an image gallery that has multiple images - click on the image to open the gallery.
Icthyosis
There are a number of forms of ichthyosis that can present in the newborn period. These are genetic disorders, typically with generalised scaling of skin. Erythroderma is a common presentation. Some babies may present as "collodion" babies.
Syndromes (e.g. Netherton's Syndrome, Sjogren-Larsson Syndrome, and Chrondrodysplasia punctata) with involvement of organs other than skin may present with ichthyosis. Some metabolic conditions may present with erythroderma with or without scaling. Staphylococcal scaled skin syndrome, congenital syphilis and other infectious diseases, as well as immunodeficiency, may present with erythroderma and scaling.
Specific investigation will depend on the diagnostic pointers provided by history and examination. It is important to ensure that the infant has adequate hydration, as hypernatraemic dyhydration may occur. General treatment of the skin is with emollients and adequate humidity. Specific treatment should be directed at the underlying cause.
Cutis Aplasia
A congenital absence of the skin. Most often it involves the scalp particularly at the vertex. Mostly singular but occasionally double or triple. They can be deeply ulcerated, or superficially eroded, or even epithelialised or scarred at birth.
They are often small defects, but very large defects may occur. Larger defects may extend to the dura or meninges. Most often, these are isolated lesions, but they may be associated with a variety of congenital anomalies, chromosomal, or genetic disorders, so that a careful physical examination of the baby is essential. Small defects will epithelialise leaving an area denuded of hair. Skin grafting should be considered for lesions larger than 3-4cm in diameter because of the risk of septic or hemorrhagic complications or venous thrombosis.
Although most often healing of an ulcerated lesion results in a flat scar, rarely, it results in a keloidal or lumpy appearance to the scar such as is seen in this 3 week old baby.
Epidermal Naevus
Epidermal naevi arise from pluripotential germinative cells in the basal layer of the embryonic epidermis. These cells give rise to keratinocytes as well as cells involved in the formation of skin appendages. Thus if the major component of the naevus is that of keratinocytes, it may be referred to as a "naevus verrucosus", if sebaceous glands "naevus sebaceous", if hair follicles "naevus comedonicus", etc.. Very few lesions are exclusively of one type and the predominant tissue may vary with the evolution of the lesion in time. This has led to a plethora of descriptive terms and a resultant terminological confusion in the literature! Most specialists in this field would refer to such lesions as "epidermal naevi".
Often, these lesions may be noted at birth but some may not develop until later childhood.
Neoplastic change may occur in some lesions (10-20%) in time, mostly but not entirely in adult life.
These lesions should be of interest to the paediatricians because of the not infrequent occurrence of other organ involvement. Thus a thorough examination in the neonatal period and clinical follow up is warranted.
The term "epidermal naevus syndrome" refers to the association of an epidermal naevus with other developmental abnormalities, particularly neurological, ocular and skeletal. Cardiac and renal abnormalities may occur as well. Lesions of the head and neck are more likely to be associated with neurological abnormalities. The presence of skin lesions other than the naevus itself such as café au lait spots, hypo or hyperpigmented lesions may occur more frequently with this syndrome and should provide the paediatrician with a warning to the possibility of its emerging in time.
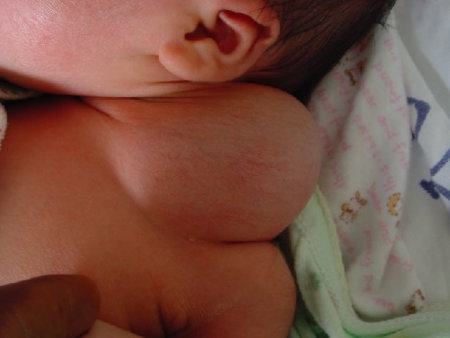
Cystic Hygroma
This is a localised lymphangioma that is typically multicystic and/or multinodular. It palpates as either a soft blubbery mass or a firmer mass or "masses" when multinodular. It commonly affects the cervicofacial region and trunk. It may rapidly enlarge and has therefore the potential of compromising the airways. Thus if antenatal diagnosis is made, the mass requires close follow up if found to be close to the airways. Treatment is either by excision or injection of a sclerosing agent.
This is not to be confused the cystic hygromas noted in early fetal life. Such lesions are often associated with chromosomal anomalies particularly Turner syndome and may be the precursor of the pterygium colli seen in some 45XO babies at birth.
Incontinentia Pigmenti
An X-linked dominant disorder with most but not all cases affecting females. The skin changes follow characteristic four stages. In the neonatal period the first stage is noted with blisters often preceded or accompanied by erythema. These involve any part of the body but usually not the face. They do not cross the midline.
These lesions are best seen in the second photograph in the groin and suprapubic region. The lesions follow a linear distribution in the limbs and circumferentially around the trunk.
Crops of lesions may occur over a period of weeks to few months. During that stage, peripheral eosinophilia may be noted. The second stage follows and is characterised by hyperkeratosis or verrucous changes. At times the 2 stages occur simultaneously as noted in the first and third photograph.
The third stage is that of hyperpigmentation typically appearing as streaks or whorls. It may be present throughout childhood. The fourth stage seen in teenage or adults is that of pale or atrophic streaks.
In the neonatal period, IP must be differentiated from herpetic lesions, bullous impetigo and epidermolysis bullosa.
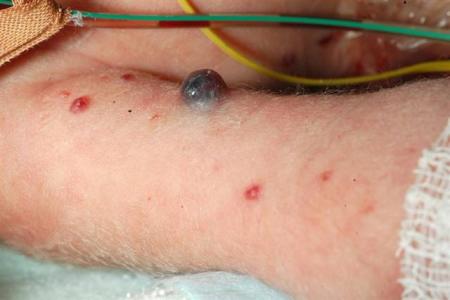
Neuroblastoma
Neuroblastoma is the most common malignant tumour presenting in neonates. It may be present at birth.
The underlying abnormality is a proliferation of neural crest cells that normally give rise to the adrenal medulla and sympathetic ganglia, and as such can occur anywhere that sympathetic neural tissue is present. Although the adrenal medulla or reteroperiteum are most commonly affected, the primary lesion is frequently not found in neonates.
The cutaneous findings may be of bluish, firm papules and nodules on the trunk and extremities. The lesions may blanch on application of pressure, thought to be due to the local release of catecholamines.
The differential diagnosis includes leukaemia, lymphoma, and causes of "blueberry muffin" lesions (such as congenital rubella or CMV infection).
Skin biopsy may be diagnostic. Other investigations that can be performed to confirm the diagnosis include elevated urinary catecholamines. Prognosis is dependent on the age of the infant and the staging of the tumour.
"Autoimmune" rash
This infant developed widespread skin lesions which appeared and disappeared in various places for few days. Some lesions had a target appearance with central pallor surrounded by an erythematous border. Others coalesced into large patches. Subsequently, the baby's mother was diagnosed with an autoimmune disorder, probably Systemic Lupus Erythematosis.
The typical skin lesions of neonatal SLE affect mostly the scalp and face, but may be more widespread. These are erythematous, scaly and sharply demarcated. However, more widespread lesions may assume the character depicted in these photographs.
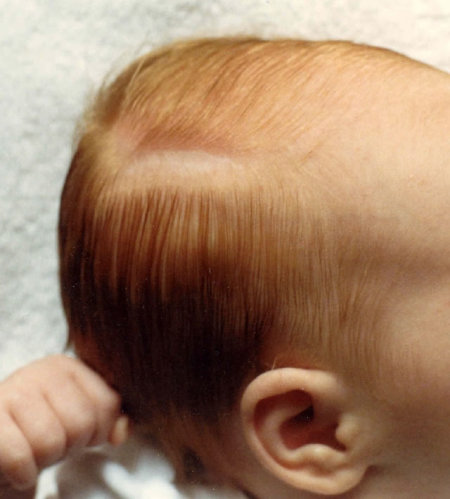
Neonatal Morphea
An extremely rare phenomenon, this infant was born with this typical lesion best described as a "coup de sabre".
The area was sclerotic with central atrophy.
It is presumed that localised scleroderma would have occurred from the passive transfer of particular autoimmune antibodies from the mother.
Subcutaneous Fat Necrosis
A rare disorder that affects the newborn in the first few weeks of life. There is often a history of a preceding stressful event such as fetal distress, asphyxia, sepsis, or hypothermia.
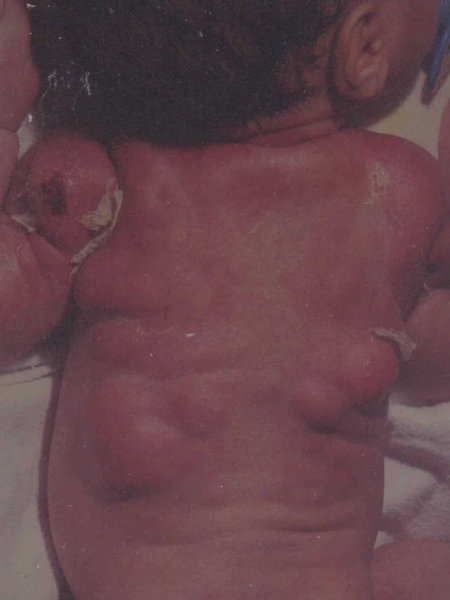
As noted in the photograph, these are well circumscribed, indurated nodules which may be tender to palpation with a reddish, sometimes purplish discoloration.
They affect areas of fat distribution such as the neck, shoulders, back and thighs.
The lesion over the left shoulder had ulcerated. Some of these lesions were drained and sterile "pus" was obtained.
This infant developed significant hypercalcaemia which is a known complication of this disorder. It was treated at the time with forced diuresis with frusemide, low calcium milk formula, and systemic steroids.
Collodion Baby
This is a rare condition, and presents with the phenotype of a baby that appears smooth and with a shiny membranous covering.
The baby may also appear dysmorphic due to contractures, the effects of the tight skin on facial features, and malformed ears.
There may be difficulties with closing the eyes (ectropion) and mouth (eclabion).
The most common causes are ichthyotic disorders (most commonly autosomal recessive ichthyosiform erythroderma or lamellar ichthyosis), but other conditions have been associated with this phenotype including Sjorgren-Larsson Syndrome and neonatal Gaucher disease.
The main issues in the neonatal period are the risk of infection associated with loss of skin integrity. Fluid balance and intravascular access are also significant challenges. Treatment is usually in a high humidity environment, and liberal use of emollients.
Polydactyly
Supernumary digits arise from the lateral surface of a digit, most commonly on the ulnar aspect of the little finger. They vary in size and shape, and can vary between being a small pedunculated nubbin of skin (as in the images to the left) through to being a complete digit containing nail and cartilage.
Although most commonly an isolated anomaly, polydactyly may be associated with other syndromes so the baby should be carefully examined for other abnormalities.
In general, if the duplicated digits are large, surgical excision is the best treatment. For pedunculated lesions, ligation may be appropriate.
Hydrocoele
Hydrocoeles are commonly present at birth, but may appear in infancy.
They present as a scrotal swelling and may be confused with an inguinal hernia. They are due to persistence of the processus vaginalis (a peritoneal projection that accompanies the testicle in its descent into the scrotum). Fluid in the hydrocoele may remain in communication with the peritoneal cavity, so the hydrocoele can change in size.
It is important to differentiate them from inguinal herniae (although the two can co-exist). However, there are many causes of inguinal swellings and abnormalities.
The images to the right demonstrate an infant with bilateral hydrocoeles, with the right larger than the left. Notice that there is some bluish discolouration of the right hemi-scrotum. The upper margins were able to be defined, the swellings were not tender, and were irreducible. The lower image shows the hydrocoele on the right transilluminated.
Umbilical Hernia
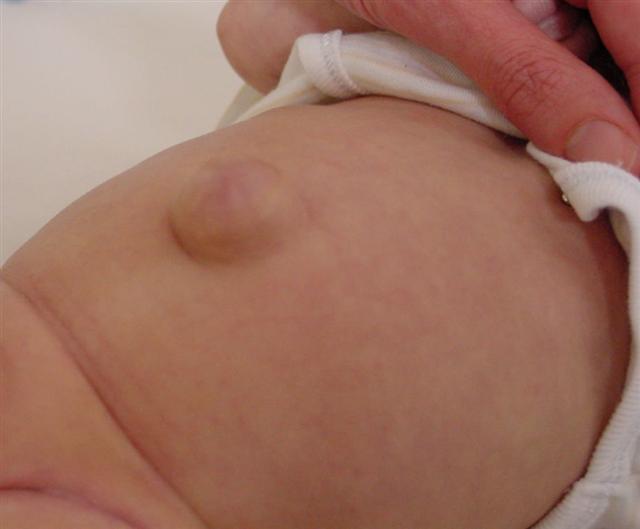
Umbilical hernias are common in infancy, occurring in as many as 1 in 6 children. They are due to incomplete closure of the ring of muscle around the umbilical ring through which the umbilical vessels enter the fetus.
They are more common in preterm infants, in children with Down Syndrome, and children with hypothyroidism. It is important to differentiate umbilical hernias from small omphalocoeles.
Most umbilical hernias close spontaneously within 3-5 years. Large hernias are less likely to close than small hernias and, as compared to inguinal hernias, incarceration is very rare. It is commonly suggested that treatments such as taping a coin to the hernia to keep it in, or strapping it, will promote resolution. Whilst unlikely to do any harm, these strategies do not have any beneficial effect. If the hernia is still present at the age of 3, referral to a paediatric surgeon is indicated.
