Benign lesions in the newborn
Please note: images that have a white symbol at the top right, such as the Erythema Toxicum Neonatorum image below, indicates an image gallery that has multiple images - click on the image to open the gallery.
Erythema Toxicum Neonatorum
Onset in the second to third day of life, mostly in term babies of lesions characterised by a central whitish to yellowish papule surrounded by a halo of erythema, mainly over the trunk but also in the limbs and face.
Lesions may intensify or coalesce particularly in response to local heat. They wax and wane over the ensuing 3 to 6 days. They are benign. Aetiology is unknown.
Milia
These commonly occur on the face and scalp, and consist of tiny white papules which are usually discrete.
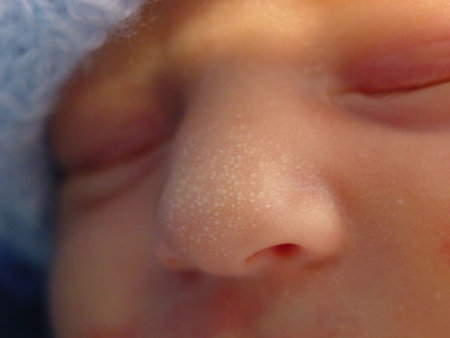
They can however occur anywhere, and may be present at birth or appear subsequently. They usually resolve within a few months without treatment.
Milia are inclusion cysts which contain trapped keratinised stratum corneum. They may rarely be associated with other abnormalities in syndromes including epidermolysis bullosa and the oro-facial-digital syndrome (type 1).
Similar lesions may be seen in the mouth in some infants. When on the hard palate, they are referred to as Epstein's pearls; when on the alveolar ridges, they are called alveolar cysts or Bohn's nodules.
Miliaria
Miliaria is due to obstruction of sweat and rupture of the eccrine sweat duct.
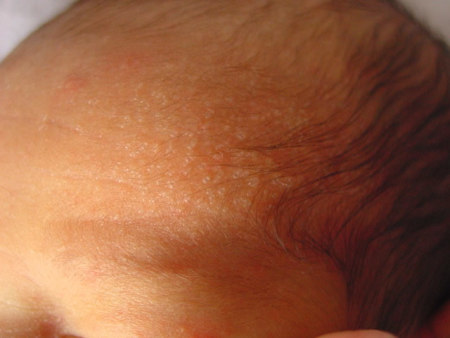
It is commonly seen secondary to thermal stress, particularly with crops of lesions over the face, scalp, and trunk. In neonates, there are two forms:
Miliaria crystallina (see image to the right), in which there are superficial vesicles which are 1-2mm in diameter. The skin does not appear inflamed.
Miliaria rubra (also called "prickly heat") results in papules and pustules from obstruction in the mid-epidermis.
It is important to ensure that the baby is not over-wrapped, and once the heat stress is removed the lesions usually resolve quickly.
Seborrhoeic Dermatitis
Seborrhoeic dermatitis primarily affects the scalp and intertriginous areas. It is most common in the first 6 weeks of life, but can occur in children up to 12 months of age.
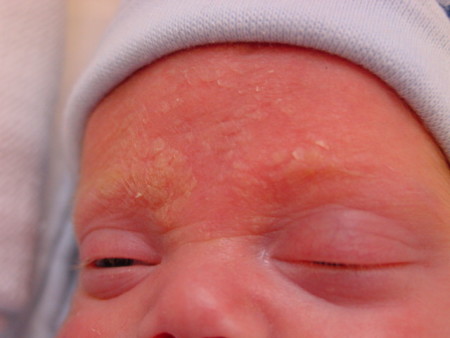
Involvement of the scalp is frequently termed "cradle cap", and manifests as greasy, yellow plaques on the scalp. Other commonly affected areas include the forehead and eyebrows (as in the photo to the right), nasolabial folds, and external ears. Involvement of skin creases, such as the nappy area, can lead to secondary Candidal infection and maceration.
The aetiology is unknown. Treatment includes the use of a mild tar shampoo, oatmeal baths, and avoidance of soaps. Occasionally, a mild topical steroid may be indicated.
Neonatal acne
Neonatal acne may be present at birth, or develop over the first 2-4 weeks of life. There is controversy over whether it is truly acne or whether it represents a form of pustular disorder in the newborn period. As a result, the term neonatal cephalic pustulosis has been mooted.
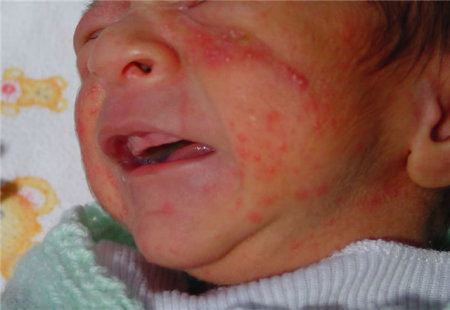
The condition consists of pustules over the cheeks primarily, but also involves other areas of the face and the scalp.
As opposed to infantile acne (which develops after 2 months) and acne of adolescence, there are no comedomes in the neonatal form. It may be difficult to differentiate between acne and miliaria rubra.
Neonatal acne resolves spontaneously and without scarring.
Nappy Rash (Diaper dermatitis)
Nappy rash is a common problem for neonates within the first few months of life. Whilst the exact aetiology of nappy rash is not clear, it is felt to be due to moisture in the nappy environment and from irritation from urine and stool.
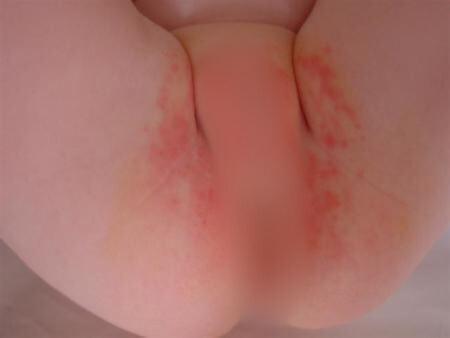
Many infants will be affected by superinfection with Candida albicans.
Typically in Candidal nappy rash, there is erythema in the perineal region, with satellite lesions which may coalesce. There is often an appearance of scale. In the images to the left from the same baby, satellite lesions are seen. Note that there are some lesions close to the umbilicus and extending around the flank. Swabs were positive for Candida.
Treatment primarily involves the use of a topical agent such as nystatin or miconazole. There should be liberal use of barrier creams, and soiled and wet nappies should be changed promptly. Oral nystatin may be used in conjunction with topical treatment, although this may not improve resolution. Occasionally, in severe cases, a mild topical steroid may be needed.
Conditions that need to be considered in the differential diagnosis include psoriasis, contact or irritant dermatitis, and zinc deficiency.
Mongolian spots
The photos show a typical Mongolian spot with bluish discoloration.
This is a very common benign skin pigmentation occurring frequently in Polynesian, Asian and Mediterranean babies but also, though to a much lesser extent, in Europeans.
Although the intergluteal area is the most common site, similar lesions may occur over the trunk or extremeties and at times multiple lesions may be noted.
Such lesions have been confused for bruises of child abuse. They gradually fade during the first few years of life.
Benign Pustular Melanosis of the Newborn
Lesions are present at birth and are characterised by superficial pustules which rupture easily without any actual pus content, leaving a spot of hyperpigmentation.
Some hyperpigmented lesions may be present at birth. Any area of the body may be involved.
The pustules last for a day or two but the pigmented spots may persist for a long time.
Aetiology is unknown. Smears from the pustules reveal polymorphonuclear leukocytes with absence of organisms.
Sucking blisters
These lesions are present at birth, most often over the dorsal and lateral aspect of the wrist. They may appear like well demarcated bruises or they may be vesicular. They can be either bilateral or unilateral. Less often, they may be noted more proximally in the forearm. The infant is noted to exhibit excessive sucking activity.
The absence of lesions in other parts of the body and the otherwise well appearance of the infant would rule out pathological disorders presenting with similar lesions.
