Curriculum
The last decade has seen tremendous advances in simulation, including a wide range of complexity and design. In order to better organise and support simulation in our organisation we have adopted and applied the Sim Zone framework of Roussin and Weinstock (2017) to the organisational curriculum.
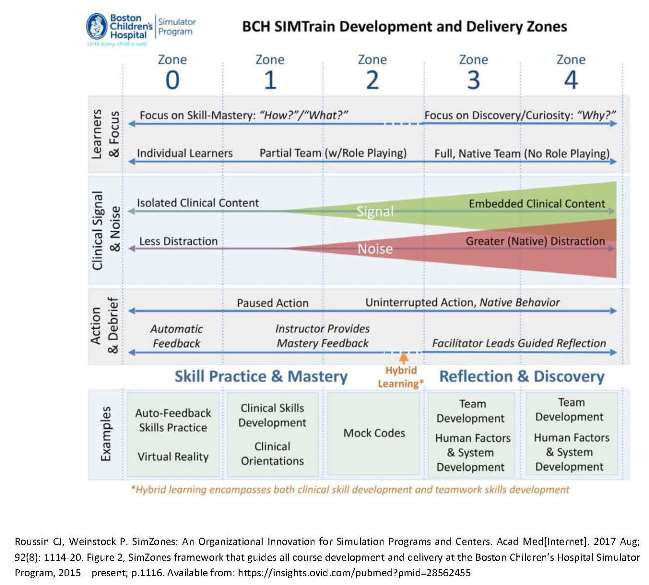
Zone 0: Skills Teaching
Zone 0 simulations involve direct teaching and corrective, automatic feedback to an individual learner. Simulation activities are focused on the acquisition of new clinical knowledge or skills in relation to specific learning objectives. Clinical content is isolated, distractions are minimised, and direction is provided during the simulation.
Zone 1: Clinical Skills and Competencies
Zone 1 simulations involve instruction to a partial clinical team (i.e nursing or medical) within a controlled patient environment. Simulation activities are focused on set clinical objectives and the application of learned foundational clinical skills through guided, experiential learning. Clinical content remains relatively isolated, distractions are lessened, and direction is provided during paused action within the simulation.
Zone 2: Scenarios
Zone 2 simulations involve situational instruction delivered at the beginning of a clinical scenario to a partial or complete clinical team. Simulation activities can occur in unfamiliar or offsite locations and are designed around set clinical learning objectives that are predominantly skills-based within a scenario to allow experiential learning. Clinical content is embedded within the scenario and distractions occur more frequently. Discussion is facilitated at the end of the simulation using the plus/delta debrief methodology and may have both a clinical and team development focus.
Zone 3: Team Training
Zone 3 simulations are delivered in situ to multidisciplinary, native clinical teams using high-fidelity manikins and adjuncts. This creates the realism that allows clinicians to explore their work environment and systems, while working as a team in time-critical events. A structured debrief is facilitated at the end of the simulation using the advocacy and inquiry methodology. This is an opportunity to engage clinical experts and explore the human factors that can impact patient outcomes.
Zone 4: Real Clinical Events
Zone 4 allows teams to debrief real events using the safe and structured framework of the After Critical Event (ACE) Review. This is an opportunity to review systems and processes in use for individuals to identify strengths and areas of concern. The information gathered informs quality and safe patient care.
