Vascular lesions in the newborn
Binary Classification of Vascular Anomalies¹
The terminology for vascular lesions has been confusing, with the same or similar terms used for different lesions with different characteristics and behaviours. In efforts to standardise terminology, the classification below was developed. "Tumors” arise by endothelial proliferation, and “malformations” are structural abnormalities that exhibit normal (slow) endothelial turnover.
| Tumours | Haemangioma Haemangioendotheliomas Angiosarcoma Miscellaneous |
| Malformations | Slow Flow - Capillary - Lymphatic - Venous Fast Flow - Arterial Combined |
Please note: images that have a white symbol at the top right, such as the haemangioma image below, indicates an image gallery that has multiple images - click on the image to open the gallery.
Haemangiomas
Haemangiomas are relatively common, occurring in up to 10% of infants by 4 weeks of age. They are more common in girls than boys, and are more common in preterm infants. They may initially be present at birth as a small "spot" or blanched area. The natural history is for them to grow over the next 6 months before gradually involuting, usually over the next few years. There is often residual telangiectasia, scarring, or loose skin despite involution over many years.
They are not usually associated with extra-cutaneous syndromes. However, midline haemangiomas (especially those over the lumbosacral area) may be associated with underlying vertebral and spinal cord anomalies. Large haemangiomas over the upper face and scalp have been associated with midline thoracic and posterior intracranial anomalies, respectively.
Most do not require any intervention or treatment. Despite their vascular origin, bleeding is rarely a problem. If they are over areas such as the eye, ear, mouth, airway, anus or urethra they can interfere with function. Oral corticosteroids are often effective at promoting resolution. Life threatening lesions may also be treated with interferon.
A single often large appearing "haemangioma" with asscociated thrombocytopenia (the Kasabach-Merritt syndrome) should raise the suspicion that one is dealing with a haemangioendothelioma rather than a haemangioma and the management of the condition will be different.
Diffuse Neonatal Haemangiomatosis
Whilst haemangiomas are common in neonates (up to 2.6%), disseminated neonatal haemangiomas are rare. This condition is apparent with multiple small and superficial haemangiomas. There may be an appearance of pallor around the lesions.
Visceral involvement occurs in around 50% of cases, but there is no particular pattern or number of cutaneous haemangiomas that either suggest or exclude visceral involvement. Some infants will manifest with high output cardiac failure, gastrointestinal haemorrhage, visceral haemorrhage, ocular involvement, or hydrocephalus. Assessment should include imaging of liver and brain. Babies require close follow-up, as mortality rates as high as 80% have been reported.
Visceral involvement per se is not an absolute indication for treatment. Systemic corticosteroids are the first line of treatment for those infants who have complications or lesions over critical structures such as the eye, ear, or mouth. Topical or intra-lesional steroids can also be used.
The last image in the gallery on the right shows multiple colour Doppler signals in the right lobe of the liver of the infant pictured. No other organ involvement was apparent in the immediate neonatal period. There was, however, rapid development of high-output cardiac failure over the next three weeks.
Port Wine Stains
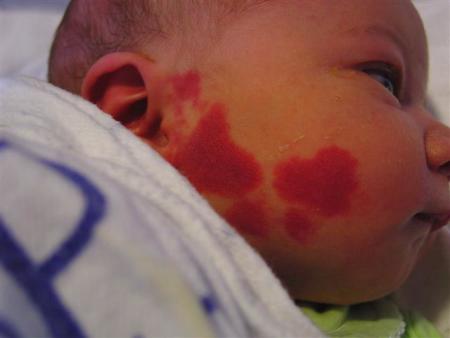
Port wine stains (PWS) are almost always evident at birth and are a capillary malformation. They are usually sporadic, although some occur in families in an apparently autosomal dominant inheritance. They are initially pink or red, and grow in proportion to infant growth. Although they may appear to lighten in the first few months, they generally darken after this.
They can be associated with other skin anomalies such as extensive mongolian spots.
An important association is Sturge-Weber syndrome: PWS involving the forehead (V1 area of the trigeminal nerve), eye abnormalities (choroidal vascular abnormalities, glaucoma), and leptomeningeal and brain abnormalities (vascular malformations, calcification, or cerebral atrophy). Another association is Klippel-Trenaunay syndrome, with a capillary malformation and overgrowth of the soft tissue and bone of the affected limb.
Treatment of PWS is possible using a laser, although improvement rather than complete resolution is most common.
Vascular Malformations
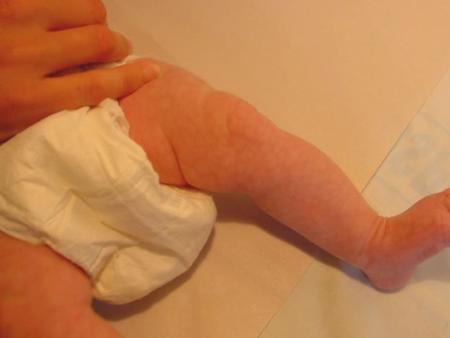
Unlike haemangiomas, vascular malformations are noted at birth. They do not have a sex predilection.
Most importantly, unlike haemangiomas the postnatal growth is not rapid but is commensurate with the overall growth of the infant, as was the case with this malformation of the arm shown in the image on the right.
Vascular lesions can be referred to the Vascular Malformation clinic at Starship Hospital
"Salmon Patches"
"Salmon patches" are seen commonly in the newborn period.
They are more common in Caucasian populations. Alternative terms are naevus simplex, "angel kisses" (when on the forehead or eyelids), and "stork bites" (over the nape of the neck). They are midline malformations consisting of ectatic capillaries in the upper dermis with normal overlying skin.
Most will resolve over the first couple of years of life, but some - especially the nuchal lesions - may persist into adulthood.
It is important to differentiate salmon patches from port-wine stains (PWS). PWS are more lateral, do not resolve, and may darken and thicken with age.
Some haemangiomas over the eyelid may also start as a faint erythematous patch before developing into a more typical haemangioma.
Cutis Marmorata
This is a reticulated pattern of constricted capillaries and venules, and is often called "mottling".
It is due to vasomotor instability in immature infants. It generally resolves with increasing age and for most infants is of no significance.
However, it may reflect underlying poor perfusion and infants who develop mottling and are unwell need to be clinically evaluated for sepsis and other illnesses.
Some infants may have localised and marked cutis marmorata (cutis marmorata telangiectatica congenita), which may be associated with other defects.
Harlequin Phenomenon
Shown at right is an excellent example of the Harlequin phenomenon in which there is striking reddening of one side of the body and blanching of the other half with a sharp line of demarcation in between.
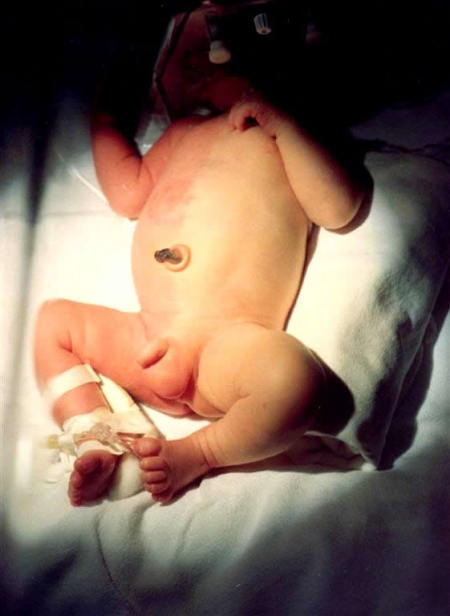
Each episode may last from seconds to minutes occasionally longer and the episodes may recur. Such episodes occur most often during the first few days of life. They are thought to be a vascular manifestation of the changes that are occurring in the autonomic system in the newborn.
Reference
Enjolras O, Mulliken JB. Vascular tumors and vascular malformations (new issues). Adv Dermatol 1997;13:375-423.
