Infective lesions in the newborn
Please note: images that have a white symbol at the top right, such as the Bullous Impegito image below, indicates an image gallery that has multiple images - click on the image to open the gallery.
Staphylococcal pustules
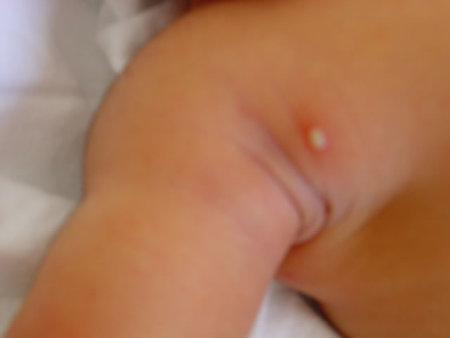
The humble superficial pustule is making a comeback with more babies being infected.
Typically, it is seen after few days of life, may affect any part of the body, but appears to have a predilection to the neck, axilla, and inguinal areas. It is almost always caused by Staphylococcus aureus.
If one lesion is seen, it may be treated "expectantly" with application of chlorhexidine mainly to prevent spread. However, if more than one lesion exists, then a course of oral antibiotic is indicated after a culture is taken. For pustules in the periumbilical area, consider at least beginning the course with systemic antibiotics.
Paronychia
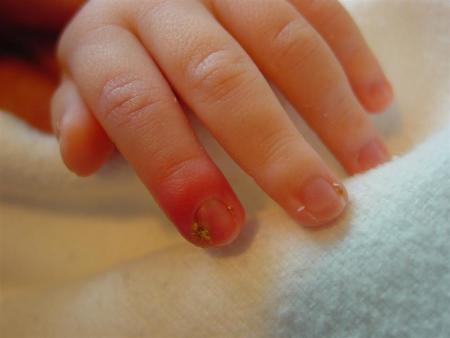
Localised inflammation of the nail fold (paronychia) is relatively common in infants. Before secondary infection (usually with Staphylococcus aureus or Streptococcus pyogenes) occurs, there is an initial separation of the skin from the nail fold. This may be exacerbated by the baby sucking their fingers or by overzealous trimming of the infant's finger nails.
Most often, the infection can be treated with oral or - in severe cases - intravenous antibiotics (our first line is usually flucloxacillin). Occasional infants may need drainage of large collections, which may be achieved by pushing the skin away from the nail fold.
For lesions that are chronic, consider Gram negative organisms or Candida as a potential cause.
Bullous impetigo
A skin infection typically caused by Staphylococcus aureus.
Lesions tend to appear in the later part of the first week of life or into the second week. Any body site may be involved with predilection to the diaper area.
The bullae are flaccid, containing straw coloured or turbid fluid, rupture easily leaving a moist denuded area. Healing occurs without scarring.
Treatment with a systemic appropriate antibiotic should be instituted particularly for lesions around the umbilicus.
Herpes simplex
Herpes simplex lesions may involve the skin, the mouth, or the eye and when they do, they provide valuable clues to the possibility of associated disseminated or CNS herpes.
Typically the lesions develop by the end of the first week or into the second week of life, as the virus is acquired at the time of birth. However, there are exceptions to the rule and occasionally lesions may be present at birth and presumably such infants would have been exposed to the virus several days prior to delivery.
Typically, grouped vesicles may be seen, often in a linear distribution if affecting the limbs such as in this photo. If the vesicle is eroded, a shallow ulcer with an erythematous base may be noted as in the second photograph.
There may be associated lesions on the lips, similar to those of the "cold sore" in the adult.
Omphalitis
Inflammation of the umbilical stump (omphalitis) most commonly occurs after day 3.
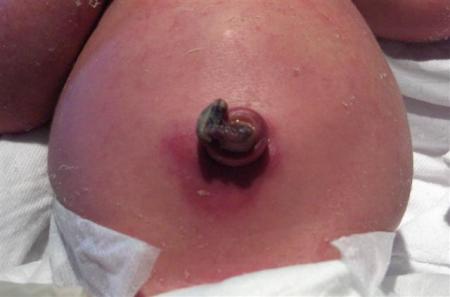
Typically the stump appears reddened and may be oedematous, with or without an exudative discharge. There may be signs of cellulitis ("cord flare") and, very rarely, fasciitis. Infective organisms are variable, but S.aureus, S.pyogenes, and Gram-negative organisms are common.
It is important to differentiate omphalitis (or funisitis - infection of the cord itself) from other causes of serous or exudative umbilical discharges, such as a persistent vitelline duct, umbilical papilloma, or urachal remnant.
Management should include a swab of the affected area for Gram-stain and culture, mainly to guide treatment. Antibiotics covering the likely organisms should be commenced. Very occasionally, infection is invasive and there can be involvement of the umbilical arteries or veins, with septic embolisation to other organs.
Skin sepsis from in utero bacterial and fungal infection
Although prolonged rupture of the amniotic membranes may result in systemic fetal and neonatal infection, the infant to the right also had generalised skin infection.
Born at 25 weeks gestation, there was a history of ruptured membranes for several days. At delivery, the baby was very foul-smelling with skin which already had evidence of infection.
Cultures from skin swabs taken at delivery grew a veritable menagerie of organisms, including Eschericia coli, Group B streptococcus, Staphylococcus aureus, and Candida albicans. The skin is desquamating and erythematous, with evidence of fissuring.
After treatment with appropriate antimicrobial agents, there was complete healing of skin at discharge with no evidence of scarring.
Congenital Syphilis
Congenital syphilis (CS) is a rare occurrence in New Zealand, although there are concerns that the reported rates of syphilis in the community appear to be increasing (Azariah S. Is syphilis resurgent in New Zealand in the 21st century? A case series of infectious syphilis presenting to the Auckland Sexual Health Service. NZMJ 2005;118(1211):U1349).
Approximately 50% of newborns with CS are asymptomatic, and cutaneous findings are not present in all symptomatic babies. Dermatological findings are quite variable, although palmar/plantar, perioral, and anogenital regions are classically described as being involved.
The images to the right demonstrate findings at birth in an affected infant, with a desquamating eruption that was widespread over the entire body. These lesions are extremely infectious. Lesions described with early disease include petechiae, haemorrhagic vesicles, bullae (pemphygis syphiliticus), and erythematous macular, papulosquamous, annular, or polymorphous eruptions. Because of the variable lesions and clinical symptoms seen with CS, it has frequently been termed "the great imitator", and it is important to consider alternative diagnoses or vesiculobullous diseases that involve the palms and soles.
Infants with CS may have extracutaneous findings such as hepatomegaly, low birth weight, thrombocytopenia, anaemia, jaundice, respiratory distress, osteochondritis, hydrops fetalis, meningitis, chorioretinitis, and pseudoparalysis. Older infants may present with "snuffles" (syphylitic rhinitis) which, in the early stages, may be mistaken for an upper respiratory tract infection.
